Peritonsillar Abscess
Peritonsillar Abscess is common so be familiar with its management - Sean M. Fox
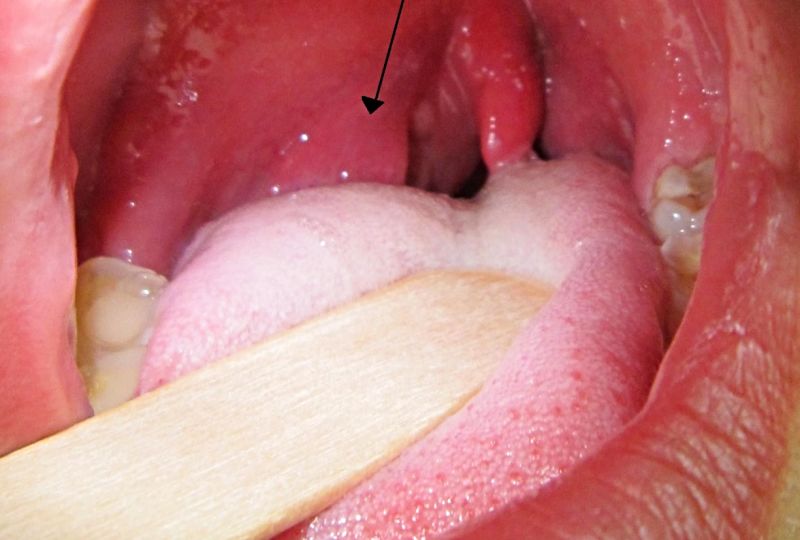
image by: James Heilman,MD
HWN Recommends
Peritonsillar abscess drainage 3.0
Dr. Michelle Lin and Dr. Demian Szyld have created great guides for the common and important emergency medicine procedure of draining a PTA (laryngoscope lighting and spinal needle for aspiration; ultrasound localization and spinal needle guard; avoiding awkward one-handed needle aspiration). This update reviews these tricks as well as some additional techniques for optimal success in draining a PTA, while avoiding the ultimate feared complication of puncturing the carotid artery.
1. Use point of care ultrasonography (POCUS)
Using the intracavitary probe provides great views of both the abscess and the nearby vessels (figure 1). Not only does it confirm…
Resources
 Peritonsillar abscess and concomitant COVID-19 in a 21-year-old male
Peritonsillar abscess and concomitant COVID-19 in a 21-year-old male
Transoral drainage of peritonsillar abscess during the COVID-19 pandemic is a high-risk procedure due to potential aerosolisation of SARS-CoV-2. This case describes conservative management of peritonsillar abscess in a 21-year-old male with COVID-19.
 Peritonsillar abscess management on the Emergency Department: conservative or surgical approach?
Peritonsillar abscess management on the Emergency Department: conservative or surgical approach?
The current literature commonly recommends surgical intervention, including needle aspiration or incision and drainage, for PTAs with success rates near 90%. However, some small studies brought novel evidence that antibiotic administration associated with steroids, pain control, and hydration can be as effective as surgical management as first-line treatment in selected in patients with mild to moderate symptoms in limited resource settings.
 Peritonsillar abscess may not always be a complication of acute tonsillitis: A prospective cohort study
Peritonsillar abscess may not always be a complication of acute tonsillitis: A prospective cohort study
Acute tonsillitis (AT) is a highly prevalent infection that is responsible for a large number of consultations. Peritonsillar abscess (PTA) is the most common deep head and neck infection, with an incidence of 10–41/100,000, and traditionally regarded as a purulent complication of AT, but the evidence for an association between the two is uncertain.
Core EM
In most textbooks, it is taught that PTA is the end-point on the pharyngitis continuum where bacterial pharyngitis progress to tonsillitis developing into peritonsillar cellulitis then ultimately abscess formation. Controversy: no real evidence to support the above proposed mechanism and there exist various inconsistencies in the above process (Passy 1994, Powell 2013) New proposed mechanism: bacterial infection of weber’s glands. Weber’s glands are a series of salivary glands that penetrate the posterior aspect of the palatine tonsillar capsule extending through the middle and distributed mainly on the superior surface of the palatine tonsils. They act to aid in the digestion of food caught in the tonsillar crypts. (Passy 1994, Powell 2013) Supporting this is the geography of abscess formation: majority of PTAs develop on the superior aspect of the tonsil.
emDocs
Most common deep neck infection in children and adolescents. Accounts for 50% of cases of deep neck infections in this population.
Distinguishing Peritonsillar Abscess from Cellulitis
Consider a few caveats when approaching the diagnosis and treatment of peritonsillar abscess in the ED. It is generally accepted that ED treatment, drainage, and outpatient follow-up is safe and effective in the vast majority of patients...Peritonsillar Abscess is common so be familiar with its management.
Peritonsillar Abscess Drainage
The Peritonsillar Abscess (PTA) is the most common deep-space infection of the head/neck, and yet drainage always seems to be easier said than done. Here’s an evidence based overview of the procedure and some tips to improve your success rate.
Tonsillitis and Peritonsillar Abscess
Peritonsillar abscess is one of the most common deep space head and neck infections in children. This collection of pus is thought to be formed most commonly as a result of spread of infection from the tonsils or the minor salivary glands of Weber, found on the superior tonsillar pole. The abscess forms deep to the tonsillar capsule between the tonsil, the superior constrictor muscle, and the palatopharyngeus muscle. The most common location is superior and medial to the tonsil; however it can occur lateral to the tonsil or even inferior
 Peritonsillar abscess drainage 3.0
Peritonsillar abscess drainage 3.0
This update reviews these tricks as well as some additional techniques for optimal success in draining a PTA, while avoiding the ultimate feared complication of puncturing the carotid artery.
American Family Physician
Peritonsillar abscess remains the most common deep infection of the head and neck. The condition occurs primarily in young adults, most often during November to December and April to May, coinciding with the highest incidence of streptococcal pharyngitis and exudative tonsillitis. A peritonsillar abscess is a polymicrobial infection, but Group A streptococcus is the predominate organism.
Harvard Health
Peritonsillar abscesses most often are found in older children, adolescents and young adults. They are less common than in the past because tonsillitis now often is treated with antibiotics, which destroy the infection-causing bacteria.
StatPearls
Peritonsillar abscesses are localized collections of pus in peritonsillar space between the tonsillar capsule and superior constrictor muscle. Since this space is composed of loose connective tissue, it is highly susceptible to abscess formation following infection. Clinical presentation may vary from acute tonsillitis with a minimal unilateral pharyngeal bulge to dehydration and sepsis.
TeensHealth
Peritonsillar abscesses usually happen as a complication of tonsillitis. If the infection breaks out of a tonsil and gets into the space around it, an abscess can form. Luckily, peritonsillar abscesses aren't that common these days because doctors use antibiotics to treat tonsillitis. Tooth and gum disease can increase the chances of a peritonsillar abscess, as can smoking — more good reasons to brush your teeth and not smoke.

Introducing Stitches!
Your Path to Meaningful Connections in the World of Health and Medicine
Connect, Collaborate, and Engage!
Coming Soon - Stitches, the innovative chat app from the creators of HWN. Join meaningful conversations on health and medical topics. Share text, images, and videos seamlessly. Connect directly within HWN's topic pages and articles.













