R/O ACS
Even without a structured scoring system, clinicians may be able to combine troponin concentrations, EKG findings, and their own “gestalt” or clinical judgement to rapidly rule out ACS - Louise A. Cullen
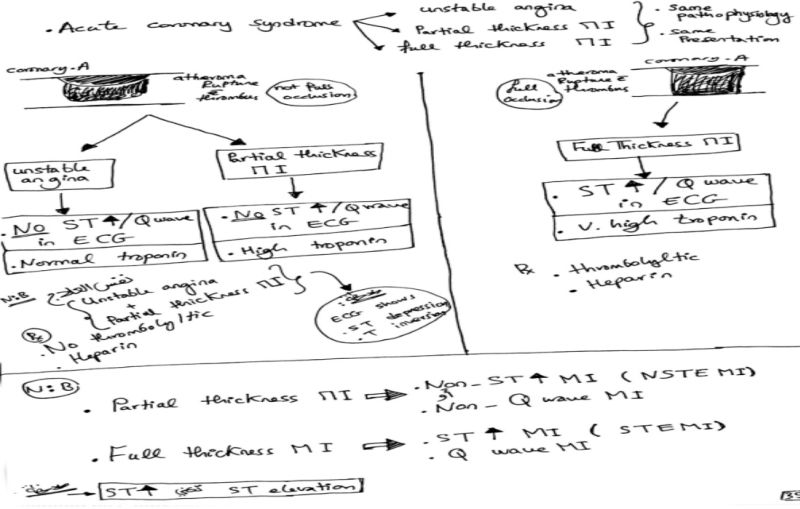
image by: Dr. mohammed.Gembry
HWN Suggests
State-of-the-Art Evaluation of Emergency Department Patients Presenting With Potential Acute Coronary Syndromes
It is well established that clinicians cannot use clinical judgment alone to determine whether an individual patient who presents to the emergency department has an acute coronary syndrome. The history and physical examination do not distinguish sufficiently between the many conditions that can cause acute chest pain syndromes. Cardiac risk factors do not have sufficient discriminatory ability in symptomatic patients presenting to the emergency department. Most patients with non–ST-segment–elevation myocardial infarction do not present with electrocardiographic evidence of active ischemia. The improvement in cardiac troponin assays, especially in conjunction with well-validated clinical decision…
Resources
 A Closer Look at the HEART Score
A Closer Look at the HEART Score
Despite popularity, there are challenges with any HEART score approach...
 Does Observation for ACS Makes Sense?
Does Observation for ACS Makes Sense?
In conclusion, observation and the interventions and tests that come with it are unlikely to help us identify ACS any better than our initial ED evaluation. Troponin will almost always become positive within 6 hours in patients with NSTEMI, so this can reasonably be identified within an ED visit.
 No Troponin, No Problem: Reimagining Chest Pain Assessment in Urgent Care
No Troponin, No Problem: Reimagining Chest Pain Assessment in Urgent Care
While the HEART score may be the most well-known clinical decision tool for chest pain presentations, its lesser-known cousin the “HEAR” or “HEAR(-T)” score has recently been externally validated with promising results. It seems the dogma of mandatory troponin testing when considering ACS may not be as ironclad as we’ve thought over recent decades—especially for the very low-risk patients.
 The Fast and the Furious: Low-Risk Chest Pain and the Rapid Rule-Out Protocol
The Fast and the Furious: Low-Risk Chest Pain and the Rapid Rule-Out Protocol
Accelerated diagnostic pathways (ADP) have been designed to identify low-risk chest pain patients in the emergency department. This review article discusses the Asia-Pacific Evaluation of Chest Pain Trial (ASPECT) score, the Accelerated Diagnostic Protocol for Chest Pain Trial (ADAPT) score, the Emergency Department Assessment of Chest Pain Score (EDACS), the HEART Score and the HEART pathway. These ADPs have been validated in various studies and aid the emergency provider with identifying the low-risk chest pain patient who is appropriate for discharge home, while at the same time highlighting those patients who would benefit from further in-patient work up.
 Troponin Testing in the Emergency Department—When 2 Become 1
Troponin Testing in the Emergency Department—When 2 Become 1
During the past 2 decades, evaluation of patients with chest pain has made a huge transition, especially with the introduction of cardiac troponin measurements and risk stratification tools.
Advantage of Using of High-Sensitivity Troponin I
High-sensitivity troponin should still be used over conventional troponin, as this allows identification of patients who are at high risk and should be followed up more closely, and may be considered of prognostic value for future events even in patients with detectable levels below the 99th percentile or with stable low-level elevations.
Can Emergency Physicians Use Clinical Gestalt to Predict Acute Coronary Syndrome?
Authors’ Conclusion: “Clinician gestalt is not sufficiently accurate or safe to either “rule in” or “rule out” ACS as a decision-making strategy.
Chest pain HPI and predictors of ACS
The simple take home point is the following: always ask your patient with chest pain if the pain radiates, if there was associated diaphoresis, if there was associated vomiting, and if the pain is associated with exertion. If the answers to any of these 4 questions is "yes," think twice before labeling the patient with a non-ACS diagnosis.
Chest Pain: Ruling Out Acute Coronary Syndrome
The 0/1-h early rule-out algorithm for ACS using high-sensitivity troponin has been prospectively validated with a NPV of 99.9%
Diagnosis and risk stratification of chest pain patients in the emergency department: focus on acute coronary syndromes
Although the new hs-cTn-based diagnostic algorithms obviate the use of clinical risk stratification scores, it is proposed to add a HEART score of 3 or less as an additional criterion for the decision on early discharge as this score predicts a very low MACE risk during early follow-up.
Does My Patient with Chest Pain Have Acute Coronary Syndrome?
Among patients with suspected ACS presenting to emergency departments, the initial history, physical examination, and electrocardiogram alone did not confirm or exclude the diagnosis of ACS. Instead, the HEART or TIMI risk scores, which incorporate the first cardiac troponin, provided more diagnostic information.”
Early Rule-Out and Rule-In Strategies for Myocardial Infarction
The challenge for clinicians is to accurately identify patients with ACS or patients at risk for ACS within 30 days while balancing the need to safely and rapidly reassure and discharge those without. Early and accurate identification of those with AMI allows prompt use of evidence-based treatments to improve outcomes in those with the condition, while improved methods to identify patients without will have important benefits both to patients and health services.
Rapid rule out of MI in the Emergency Department: a politically inconvenient innovation?
Previously, patients presenting with chest pain often represented a relatively straightforward cohort of patients who, if suspected for an ACS, would warrant automatic admission. The advent of high-sensitivity troponin now permits the risk-stratification, decision-making and discharge of these patients from the ED rather than downstream under medical or cardiology teams.
Risk Stratification of the ACS Patient in the Emergency Department and Initial Medical Therapy
The primary pitfall of ACS risk stratification and evaluation is to not consider the diagnosis in the first place. The literature suggests we inadvertently send home 1%-4% of AMI patients from the ED. Atypical presentations in the elderly, females, and diabetics can fail to alert the clinician to the possibility of ACS. A reasonable index of suspicion should be maintained for the possibility that the 60 year old with nausea and vague malaise is actually experiencing myocardial ischemia.
Ruling Out Acute Coronary Syndrome in Patients With Chest Pain
ACS is a common and potentially lethal problem. However, only about 10% of patients who present to an emergency department with chest pain actually have ACS.
The predictive value of HEART score for acute coronary syndrome and significant coronary artery stenosis
HEART score was a fair predictor of ACS and SCS in ED patients who presented with chest symptoms and were admitted to the cardiology department. The predictive power of HEART score was better for SCS than for ACS.
What decides the suspicion of acute coronary syndrome in acute chest pain patients?
Although the ECG may theoretically be the most important diagnostic tool in chest pain patients with possible ACS, the present results indicate that ED physicians do not use the ECG in this way. Instead, the physicians used symptoms as the most important assessment tool, and applied primarily the symptoms to determine the level of suspicion of ACS and to rule out ACS. The ECG was only primarily used to rule in ACS, whereas the TnT level in general played a minor role for the ACS likelihood.
 State-of-the-Art Evaluation of Emergency Department Patients Presenting With Potential Acute Coronary Syndromes
State-of-the-Art Evaluation of Emergency Department Patients Presenting With Potential Acute Coronary Syndromes
It is well established that the clinician cannot use clinical judgment alone to determine whether an individual patient who presents to the ED has an ACS. The improvement in cTn assays, especially in conjunction with clinical decision algorithms, now enables the clinician to rapidly exclude myocardial infarction.

Introducing Stitches!
Your Path to Meaningful Connections in the World of Health and Medicine
Connect, Collaborate, and Engage!
Coming Soon - Stitches, the innovative chat app from the creators of HWN. Join meaningful conversations on health and medical topics. Share text, images, and videos seamlessly. Connect directly within HWN's topic pages and articles.













